Acute Pancreatitis Symptoms: A Complete Guide to Recognizing the Warning Signs
What Is Acute Pancreatitis?
Acute pancreatitis is a sudden inflammation of the pancreas — a large glandular organ located behind the stomach — that can range from mild discomfort to a life-threatening medical emergency. Understanding acute pancreatitis symptoms is critical because early recognition can dramatically improve outcomes, reduce complications, and in severe cases, save lives.
The pancreas serves two vital functions in the human body: it produces digestive enzymes that break down food in the small intestine, and it secretes hormones like insulin and glucagon that regulate blood sugar. When the pancreas becomes inflamed, these digestive enzymes — which are normally inactive until they reach the intestine — become activated prematurely inside the pancreas itself. This leads to the organ essentially beginning to digest itself, causing the pain and damage that defines acute pancreatitis.
Each year, approximately 300,000 people in the United States are hospitalized with acute pancreatitis, making it one of the most common gastrointestinal conditions requiring hospital care. Worldwide, incidence rates have been rising steadily, partly due to increasing rates of gallstones and alcohol consumption — the two leading causes of the condition.
This guide provides a thorough, medically grounded overview of acute pancreatitis symptoms, how they develop, how they differ based on severity, what complications can arise, and when you should seek emergency medical attention.
The Hallmark Symptom: Severe Upper Abdominal Pain
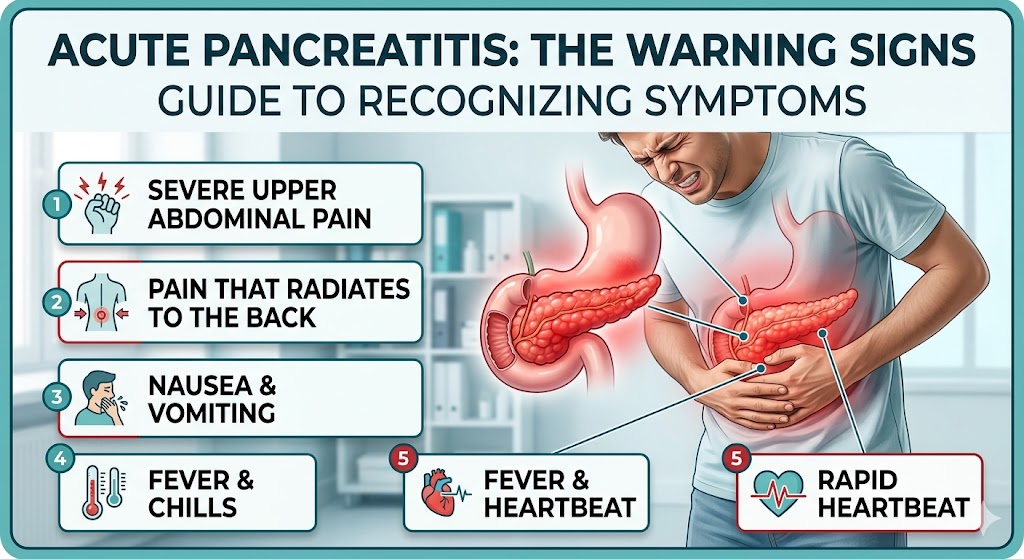
The most defining and consistent symptom of acute pancreatitis is sudden, severe pain in the upper abdomen. This pain is typically centered in the epigastric region — the area just below the breastbone and above the navel — and is often described by patients as the worst pain they have ever experienced. Understanding the specific characteristics of this pain is key to identifying acute pancreatitis quickly.
The pain usually begins abruptly and may escalate rapidly over the course of 15 to 30 minutes, reaching a peak intensity that can be incapacitating. Unlike some other abdominal conditions where pain comes and goes in waves, the pain of acute pancreatitis tends to be constant and unrelenting. Patients often describe it as a deep, boring, or gnawing sensation. Some find mild relief by leaning forward or curling into a fetal position.
One of the most diagnostically significant features of pancreatic pain is its radiation pattern. In a substantial proportion of patients — estimated at around 50% — the pain radiates to the back, particularly between the shoulder blades or to the mid-back region. This band-like quality of pain, wrapping from the front of the abdomen around to the back, is a classic hallmark that clinicians specifically look for when evaluating potential pancreatitis cases.

Nausea and Vomiting: Common Accompanying Symptoms
Nausea and vomiting are among the most frequently reported acute pancreatitis symptoms, occurring in the vast majority of patients. These symptoms typically develop alongside or shortly after the onset of abdominal pain and can be quite severe. Importantly, vomiting in acute pancreatitis does not relieve the abdominal pain — a key distinguishing feature from other causes such as food poisoning or gastroenteritis, where patients often feel better after vomiting.
The persistence of nausea and vomiting can contribute significantly to dehydration, which itself worsens the condition. When the body cannot retain fluids, blood pressure may drop, kidney function can be impaired, and the body's ability to manage the inflammatory response is compromised. This is why intravenous fluid replacement is one of the first and most critical interventions in hospital treatment of acute pancreatitis.
Patients may also experience a complete loss of appetite. The idea of eating or drinking anything is deeply unappealing during an acute attack, and eating typically worsens the pain because ingesting food stimulates the pancreas to produce more digestive enzymes, intensifying the inflammatory cycle.
Fever and Elevated Heart Rate
Systemic symptoms such as fever and an elevated heart rate (tachycardia) are common in acute pancreatitis and reflect the body's broader inflammatory response to pancreatic injury. A low-grade fever — typically between 100°F and 102°F — is present in many cases of mild to moderate acute pancreatitis. However, high fever, especially when combined with chills and rigors, may indicate a more serious complication such as infected pancreatic necrosis or systemic infection (sepsis).
Tachycardia — a heart rate above 100 beats per minute — often accompanies the pain response and can also result from dehydration and volume depletion caused by vomiting and fluid shifts into the inflamed tissue around the pancreas. Healthcare providers use heart rate and fever as important triage indicators when assessing the severity of acute pancreatitis. They are incorporated into several validated scoring systems — including the Ranson Criteria and the BISAP Score — used to predict which patients are most likely to experience severe disease.
Abdominal Tenderness and Distension
When a physician examines a patient with acute pancreatitis, they will typically find significant tenderness in the upper abdomen upon palpation. This tenderness is often severe enough that even gentle pressure causes intense pain. In more severe cases, guarding — an involuntary tightening of the abdominal muscles — and rigidity may be present, suggesting peritoneal irritation.
Abdominal distension (bloating or swelling of the abdomen) is another common finding. This occurs because inflammation causes local swelling in surrounding tissues and the associated ileus (a temporary paralysis of the bowel) causes gas to accumulate in the intestines. Patients often describe their abdomen as feeling full, tight, or swollen, and visible distension may be apparent on inspection.
Bowel sounds may be diminished or absent on auscultation, further reflecting the associated ileus. Constipation and an inability to pass gas are also frequently reported, compounding the patient's discomfort and signaling the widespread disruption that pancreatic inflammation causes throughout the digestive system.

Jaundice: A Warning Sign of Biliary Involvement
Jaundice — a yellowing of the skin and the whites of the eyes — is an important symptom to be aware of, though it is not present in all cases of acute pancreatitis. Its presence typically indicates that the bile duct has become obstructed. This is particularly relevant in gallstone-induced pancreatitis, where a gallstone lodged at the junction of the bile duct and the pancreatic duct can cause both conditions simultaneously.
When bile cannot flow freely from the liver through the bile duct into the small intestine, bilirubin — a yellow pigment produced from the breakdown of red blood cells — builds up in the bloodstream. Patients may also notice that their urine turns dark (tea-colored) and their stools become pale or clay-colored. Jaundice in the context of acute pancreatitis requires prompt medical evaluation and may indicate the need for an endoscopic procedure (ERCP) to remove the obstructing stone.
Signs of Severe Acute Pancreatitis
While approximately 80% of acute pancreatitis cases are mild and resolve within a few days with supportive care, roughly 20% progress to severe disease with potentially life-threatening complications. Severe acute pancreatitis is associated with organ failure — most commonly affecting the lungs, kidneys, and cardiovascular system. Patients may experience difficulty breathing as fluid accumulates in the lungs or around them.
Two rare but diagnostically significant skin findings can appear in cases of necrotizing pancreatitis. Cullen's sign refers to bluish-purple discoloration around the navel, while Grey Turner's sign describes similar discoloration along the flanks (sides of the abdomen). Both signs indicate that blood and inflammatory fluid have dissected through the retroperitoneal space and tracked to the skin surface, and their presence is associated with a significantly worse prognosis.
Pancreatic necrosis — the death of pancreatic tissue — can become infected, resulting in high fever, rigors, persistent abdominal pain, and signs of sepsis including confusion, rapid breathing, and extremely low blood pressure. This complication requires urgent intervention, including antibiotics and often drainage or surgical debridement.
Symptoms Based on Underlying Cause
The presenting symptoms of acute pancreatitis can vary somewhat depending on the underlying cause. In gallstone pancreatitis — the most common cause in women and overall — pain may come on suddenly and be accompanied by jaundice, with symptoms sometimes following a high-fat meal that stimulates gallbladder contraction. In alcohol-induced pancreatitis — more common in men — pain typically appears 12 to 48 hours after a binge drinking episode.
In hypertriglyceridemia-induced pancreatitis, patients may present with xanthomas (yellowish deposits under the skin) or lipemia retinalis in addition to standard pancreatitis symptoms. Identifying the underlying cause is critical for both acute management and long-term prevention of recurrence.
How Acute Pancreatitis Is Diagnosed
Diagnosis of acute pancreatitis is based on a combination of clinical presentation, laboratory tests, and imaging studies. According to the revised Atlanta Classification, a diagnosis requires at least two of the following three criteria: characteristic abdominal pain (severe epigastric pain, often radiating to the back); serum lipase or amylase levels at least three times the upper limit of normal; and characteristic findings on imaging such as CT scan or ultrasound.
Blood tests are the first line of investigation. Serum lipase is the preferred marker because it remains elevated longer than amylase and is more specific to the pancreas. An abdominal ultrasound is typically performed early in the evaluation to identify gallstones as a potential cause. A CT scan with contrast is the gold standard imaging modality for assessing severity, identifying pancreatic necrosis, and detecting local complications such as fluid collections, abscesses, or pseudocysts.

When to Seek Emergency Care
Certain acute pancreatitis symptoms demand immediate medical attention. Seek emergency care if you experience severe upper abdominal pain that comes on suddenly and does not improve; abdominal pain accompanied by fever, chills, or jaundice; persistent vomiting that prevents you from keeping down fluids; signs of shock such as extreme dizziness, fainting, or very low blood pressure; difficulty breathing or chest pain; or confusion or altered mental status.
Even if you have had pancreatitis before and recognize the symptoms, a new attack should always be evaluated medically. The severity can vary between episodes, and complications can develop rapidly. Do not attempt to manage acute pancreatitis at home without medical guidance.
Understanding Severity: Mild, Moderate, and Severe
Acute pancreatitis exists along a spectrum of severity, and symptoms can differ significantly based on where a patient falls on that spectrum. Mild acute pancreatitis — characterized by no organ failure and no local or systemic complications — typically resolves within 3–5 days with basic supportive care including IV fluids, pain management, and bowel rest. Moderately severe acute pancreatitis involves either transient organ failure or local complications such as peripancreatic fluid collections.
Severe acute pancreatitis, which accounts for roughly 5–10% of all cases, involves persistent organ failure affecting one or more organ systems and carries a mortality rate that can reach 30–50% in complicated cases. Early identification of patients at risk for severe disease — using clinical scoring systems, laboratory markers like C-reactive protein, and imaging — is essential for escalating care before organ failure becomes irreversible.
Recovery and Long-Term Outlook
For the majority of patients, acute pancreatitis symptoms resolve within a week or two with appropriate hospital treatment. The standard approach involves aggressive IV fluid resuscitation, effective pain management, nutritional support (early enteral feeding is now preferred over strict bowel rest in most guidelines), and treatment of the underlying cause. Most patients with mild acute pancreatitis are discharged within 3–7 days and return to normal activities relatively quickly.
However, patients who have experienced acute pancreatitis are at risk of recurrence, particularly if the underlying cause — whether gallstones, alcohol use, or elevated triglycerides — is not addressed. Gallstone pancreatitis carries a 30–60% risk of recurrence if the gallbladder is not removed (cholecystectomy). Repeated episodes of acute pancreatitis can lead to chronic pancreatitis — a long-term condition characterized by permanent structural damage to the pancreas, chronic pain, malabsorption, and diabetes.
Conclusion
Acute pancreatitis is a serious, potentially life-threatening condition whose symptoms — above all, the characteristic severe upper abdominal pain radiating to the back — demand swift recognition and medical response. From the hallmark pain and nausea to the more alarming signs of fever, jaundice, and organ dysfunction, being informed about the full spectrum of acute pancreatitis symptoms empowers patients, families, and caregivers to act quickly and seek appropriate care. Early intervention significantly reduces the risk of severe complications. If you or someone you know experiences symptoms consistent with acute pancreatitis, seek emergency medical evaluation immediately.