Causes of Pancreatitis: Understanding Why Your Pancreas Becomes Inflamed
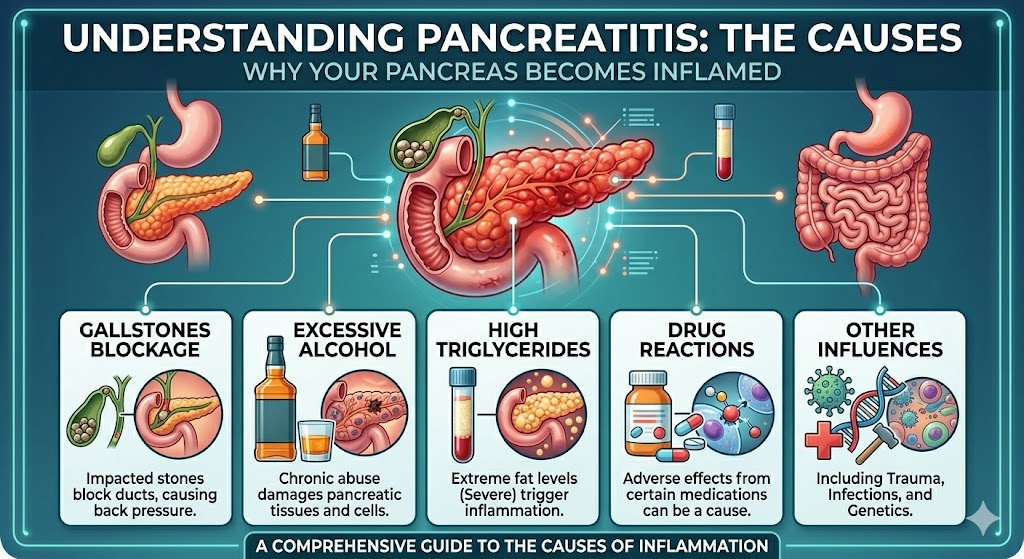
Understanding the Pancreas and Why It Becomes Inflamed
The pancreas is a remarkable organ tucked behind the stomach in the upper left abdomen, roughly six inches long and shaped like a tadpole. It works continuously to support two of the body's most vital systems: it manufactures digestive enzymes that break down fats, proteins, and carbohydrates in the small intestine, and it produces hormones — most critically insulin and glucagon — that regulate blood glucose levels. When the pancreas is healthy, these functions proceed seamlessly, entirely unnoticed by the person they sustain.
Pancreatitis occurs when the pancreas becomes inflamed, causing the digestive enzymes that it produces to become activated before they reach the small intestine. Instead of breaking down food in the intestine, these enzymes begin attacking the pancreatic tissue itself, triggering a destructive inflammatory cascade. The result ranges from a painful but temporary condition (acute pancreatitis) to a progressive, debilitating disease (chronic pancreatitis) that permanently damages the organ over time.
Understanding the causes of pancreatitis is essential not only for patients who have already been diagnosed, but also for anyone seeking to protect their long-term pancreatic health. Many of the most common causes are preventable or modifiable, meaning that with the right knowledge, people can meaningfully reduce their risk. This comprehensive guide explores every major cause of pancreatitis — from the most common culprits to the rarest triggers — with a focus on the underlying biological mechanisms that explain why each factor leads to inflammation.
Gallstones: The Leading Cause of Acute Pancreatitis
Gallstones are the single most common cause of acute pancreatitis, accounting for approximately 40–70% of all cases worldwide. Gallstones are hardened deposits of digestive fluid — primarily made of cholesterol or bilirubin — that form in the gallbladder. Under normal circumstances, the bile produced by the liver travels through the bile duct and enters the small intestine, where it helps to emulsify fats. The pancreatic duct, which carries digestive enzymes from the pancreas, joins the bile duct at the ampulla of Vater just before entering the small intestine.
When a gallstone becomes lodged at this junction, it blocks the outflow of pancreatic enzymes. The resulting backpressure causes enzymes to accumulate within the pancreatic duct, eventually triggering premature activation and autodigestion of the pancreas. This is the mechanism underlying gallstone pancreatitis. The condition is particularly common in women and in individuals who are overweight, pregnant, or over 40 — all demographic groups with higher rates of gallstone formation.
Risk factors for gallstone formation include obesity, rapid weight loss, a high-fat diet low in fiber, female sex (estrogen increases cholesterol secretion into bile), multiparity (multiple pregnancies), certain medications including oral contraceptives and cholesterol-lowering drugs, and genetic predisposition. Cholecystectomy (surgical removal of the gallbladder) is the definitive treatment for gallstone pancreatitis and is recommended to prevent recurrence.

Alcohol Use: The Second Most Common Cause
Chronic and heavy alcohol consumption is the second leading cause of pancreatitis, responsible for approximately 30% of all cases in Western countries. Unlike gallstone pancreatitis, which typically causes a single acute episode, alcohol-related pancreatitis tends to develop after years of heavy drinking and is more likely to progress to chronic pancreatitis with irreversible damage to the gland.
The exact mechanism by which alcohol causes pancreatitis is complex and not fully elucidated, but several pathways have been identified. Alcohol and its metabolites (particularly acetaldehyde) directly injure pancreatic acinar cells — the cells that produce digestive enzymes. This injury promotes premature enzyme activation within the pancreas. Alcohol also increases the protein content of pancreatic juice and reduces its bicarbonate content, making it more likely for proteins to precipitate and form plugs that block small pancreatic ducts. Additionally, alcohol sensitizes the pancreas to injury from other triggers and promotes oxidative stress and inflammation.
It is important to note that not everyone who drinks heavily develops pancreatitis — only 2–5% of heavy drinkers do, suggesting that genetic susceptibility plays a significant modifying role. However, the risk increases substantially with the quantity and duration of alcohol consumption, with heavy drinkers (more than 5 drinks per day) carrying the highest risk. The type of alcohol consumed (beer, wine, or spirits) does not appear to matter — total ethanol intake is the relevant variable.
Hypertriglyceridemia: Elevated Blood Fats as a Cause
Hypertriglyceridemia — abnormally high levels of triglycerides (fats) in the blood — is the third most common cause of acute pancreatitis, accounting for 1–14% of cases in various studies. The risk of pancreatitis becomes significant when serum triglyceride levels exceed 1,000 mg/dL (normal is below 150 mg/dL), and it rises sharply above 2,000 mg/dL. At these extreme levels, triglyceride-rich lipoprotein particles are thought to be hydrolyzed by pancreatic lipase within the pancreatic capillaries, releasing toxic free fatty acids that damage blood vessel walls and trigger inflammation.
Hypertriglyceridemia can be primary (caused by inherited genetic disorders such as familial hypertriglyceridemia or lipoprotein lipase deficiency) or secondary (caused by conditions such as poorly controlled diabetes, hypothyroidism, kidney disease, and pregnancy). It can also be exacerbated by medications including corticosteroids, thiazide diuretics, beta-blockers, antiretrovirals, and tamoxifen, as well as by alcohol consumption and a high-fat diet. Management focuses on aggressively lowering triglyceride levels through dietary modification, fibrate medications, and addressing underlying causes.
Medications: A Frequently Overlooked Cause
Drug-induced pancreatitis accounts for approximately 0.1–2% of all pancreatitis cases, but it is frequently underrecognized because clinicians may not immediately consider medication as the culprit. Over 500 drugs have been associated with pancreatitis, though for many the evidence is based only on case reports. The mechanisms vary widely: some drugs directly damage pancreatic cells, others cause hypertriglyceridemia, some promote gallstone formation, and others trigger immune-mediated reactions.
The medications most consistently linked to pancreatitis include: azathioprine and 6-mercaptopurine (immunosuppressants used in inflammatory bowel disease and transplantation); didanosine and other nucleoside reverse transcriptase inhibitors used in HIV treatment; valproic acid (an anticonvulsant); tetracycline antibiotics; sulfonamides; furosemide (a diuretic); estrogens; corticosteroids; angiotensin-converting enzyme (ACE) inhibitors; and GLP-1 receptor agonists such as exenatide (though the evidence for the latter remains debated). Identifying and discontinuing the offending drug is the cornerstone of management for drug-induced pancreatitis.

Genetic and Hereditary Causes of Pancreatitis
Genetic factors play an important role in pancreatitis, both as direct causes and as modifiers of risk from environmental triggers. Hereditary pancreatitis is a rare autosomal dominant condition most often caused by mutations in the PRSS1 gene (which encodes cationic trypsinogen), leading to premature and unregulated trypsin activation within the pancreas. Individuals with hereditary pancreatitis typically present with recurrent episodes of acute pancreatitis beginning in childhood or early adulthood and have a markedly elevated lifetime risk of developing chronic pancreatitis and pancreatic cancer.
Mutations in the SPINK1 gene (serine protease inhibitor Kazal type 1), which encodes a trypsin inhibitor that provides a safety mechanism against premature enzyme activation, are found in a subset of patients with idiopathic (unknown cause) pancreatitis. CFTR gene mutations — the same mutations associated with cystic fibrosis — are overrepresented among patients with chronic idiopathic pancreatitis, even in individuals without classic cystic fibrosis symptoms. CTRC gene mutations, affecting chymotrypsin C (another protective enzyme), have also been identified as genetic risk factors.
Genetic testing is increasingly available and recommended for patients with unexplained recurrent pancreatitis, early-onset disease, or a family history of pancreatic disease. Identification of a genetic cause has important implications for counseling, surveillance for complications (including pancreatic cancer), and management decisions.
Autoimmune Pancreatitis: An Immune-Mediated Cause
Autoimmune pancreatitis (AIP) is a distinctive form of pancreatitis caused by an aberrant immune response against the pancreas. It is increasingly recognized as a cause of both acute and chronic pancreatic inflammation and accounts for about 2–5% of chronic pancreatitis cases. There are two types: Type 1 AIP, the more common form, is associated with elevated serum IgG4 levels and is part of a systemic IgG4-related disease that can affect multiple organs; Type 2 AIP is a pancreas-specific condition not associated with IgG4 but linked to inflammatory bowel disease.
AIP typically presents with painless obstructive jaundice (mimicking pancreatic cancer), diffuse pancreatic enlargement on imaging, and elevated serum IgG4 (in Type 1). It responds dramatically to corticosteroid therapy, which is both diagnostic and therapeutic. Correctly diagnosing AIP is critically important because it is often mistaken for pancreatic cancer, potentially leading to unnecessary surgery.
Hypercalcemia: High Blood Calcium as a Cause
Hypercalcemia — abnormally elevated blood calcium levels — is a less common but well-established cause of pancreatitis, accounting for approximately 1–2% of cases. The most common causes of hypercalcemia include primary hyperparathyroidism (excess parathyroid hormone production), malignancy (cancer releasing calcium from bones), vitamin D toxicity, and granulomatous diseases such as sarcoidosis. High calcium levels damage pancreatic acinar cells and activate trypsinogen within the pancreas, triggering the inflammatory cascade.
Pancreatitis related to hypercalcemia may be difficult to identify without routine blood chemistry testing, as calcium levels are not typically assessed in every patient presenting with abdominal pain. Treating the underlying cause of hypercalcemia (for example, removing a parathyroid adenoma in primary hyperparathyroidism) resolves the metabolic abnormality and prevents further episodes of pancreatitis.
Anatomical and Structural Causes
Certain structural abnormalities of the pancreatic and biliary ductal system can predispose individuals to recurrent pancreatitis. Pancreas divisum is the most common congenital anomaly of the pancreas, occurring in approximately 5–10% of the population. In this condition, the two parts of the embryonic pancreas fail to fuse during development, leaving the majority of the pancreatic tissue draining through a small minor papilla that may be inadequate to handle the full volume of pancreatic secretions, particularly during periods of high stimulation.
Annular pancreas is a rare anomaly in which a ring of pancreatic tissue surrounds and may compress the duodenum. Choledochocele (a cystic dilation of the intramural portion of the bile duct) and various other ductal abnormalities can also obstruct pancreatic outflow and cause inflammation. Sphincter of Oddi dysfunction — a functional or structural abnormality of the muscular valve controlling the junction of the bile duct and pancreatic duct — is another proposed cause of recurrent pancreatitis, particularly in patients who have previously had their gallbladder removed.

Infections as a Cause of Pancreatitis
While infections are a less common cause of pancreatitis compared to gallstones and alcohol, various viral, bacterial, and parasitic infections can trigger pancreatic inflammation. Among viruses, mumps was historically the most well-known cause of viral pancreatitis, though vaccination has made this rare in developed countries. Other viruses implicated in pancreatitis include Coxsackievirus B, cytomegalovirus (CMV), Epstein-Barr virus, hepatitis B and C, HIV, and, more recently, SARS-CoV-2 (COVID-19), which has been associated with pancreatic injury in some patients.
Bacterial infections causing pancreatitis are less common but include Mycoplasma pneumoniae, Salmonella, Leptospira, and Legionella species. Parasitic infections — particularly Ascaris lumbricoides (roundworms), which can migrate into the bile duct and obstruct the ampulla of Vater — are an important cause of pancreatitis in regions where this parasite is endemic.
Trauma and Iatrogenic Causes
Physical injury to the abdomen — whether from blunt trauma (such as a car accident or sports injury) or penetrating wounds — can directly damage the pancreas and cause pancreatitis. Blunt abdominal trauma is a particularly common cause of pancreatitis in children, as the relatively smaller abdominal cavity and less developed musculature provide less protection to the pancreas. The characteristic injury is a pancreatic contusion or laceration at the body of the pancreas, which lies just anterior to the vertebral column.
Post-ERCP pancreatitis is the most common serious complication of endoscopic retrograde cholangiopancreatography (ERCP) — a procedure used to treat bile duct stones and other conditions — occurring in 3–10% of all ERCP procedures. It results from mechanical trauma to the papilla, hydrostatic injury from contrast injection, thermal injury from electrocautery, and enzyme activation. Post-surgical pancreatitis can also occur following procedures involving the pancreas, duodenum, bile duct, or even distant organs, particularly cardiac surgery with cardiopulmonary bypass.
Idiopathic Pancreatitis: When No Cause Can Be Found
Despite thorough investigation, the cause of pancreatitis cannot be identified in approximately 15–25% of cases, classified as idiopathic pancreatitis. However, advances in diagnostic technology — including endoscopic ultrasound (EUS), genetic testing, and advanced lipid profiling — have progressively reduced this proportion by uncovering previously hidden causes such as microlithiasis (tiny gallstones or biliary crystals too small to detect on standard ultrasound), genetic mutations, subtle ductal anomalies, and early autoimmune disease.
In many cases of apparent idiopathic pancreatitis, microlithiasis — microscopic crystals of cholesterol or calcium bilirubinate in the bile — is found to be the responsible culprit when bile is microscopically examined after collection during ERCP. This discovery has led some gastroenterologists to recommend cholecystectomy or ursodeoxycholic acid therapy even in patients without demonstrable gallstones on standard imaging.
Preventing Pancreatitis: Addressing Modifiable Causes
Many of the leading causes of pancreatitis are modifiable, making prevention a realistic and important goal. The most impactful preventive strategies include maintaining a healthy body weight to reduce gallstone risk; limiting or eliminating heavy alcohol consumption; managing blood triglyceride and cholesterol levels through diet, exercise, and medication when needed; and carefully reviewing any new medications with a healthcare provider for their potential to cause pancreatitis, especially in patients with prior pancreatic disease.
For patients who have experienced gallstone pancreatitis, timely cholecystectomy is the most important preventive measure. For those with hereditary or genetic causes, regular monitoring and avoidance of additional risk factors (particularly alcohol) can slow progression and reduce the frequency of attacks. Smoking — while not a direct cause of pancreatitis — has been identified as an independent risk factor for both acute and chronic pancreatitis and for progression of chronic pancreatitis, and cessation is strongly advised.
Conclusion
Pancreatitis is a complex condition with a wide spectrum of causes, ranging from common and easily identifiable triggers like gallstones and alcohol to rare genetic disorders and structural abnormalities. Understanding the specific cause of pancreatitis in each patient is essential for directing appropriate treatment, preventing recurrence, and managing long-term risk. If you have experienced pancreatitis or have risk factors for the condition, work closely with your healthcare provider to identify any modifiable contributors and implement a personalized prevention plan. With the right approach, many causes of pancreatitis are preventable — and the quality of life for those already affected can be substantially improved through targeted management.