Signs of Pancreatitis You Should Never Ignore
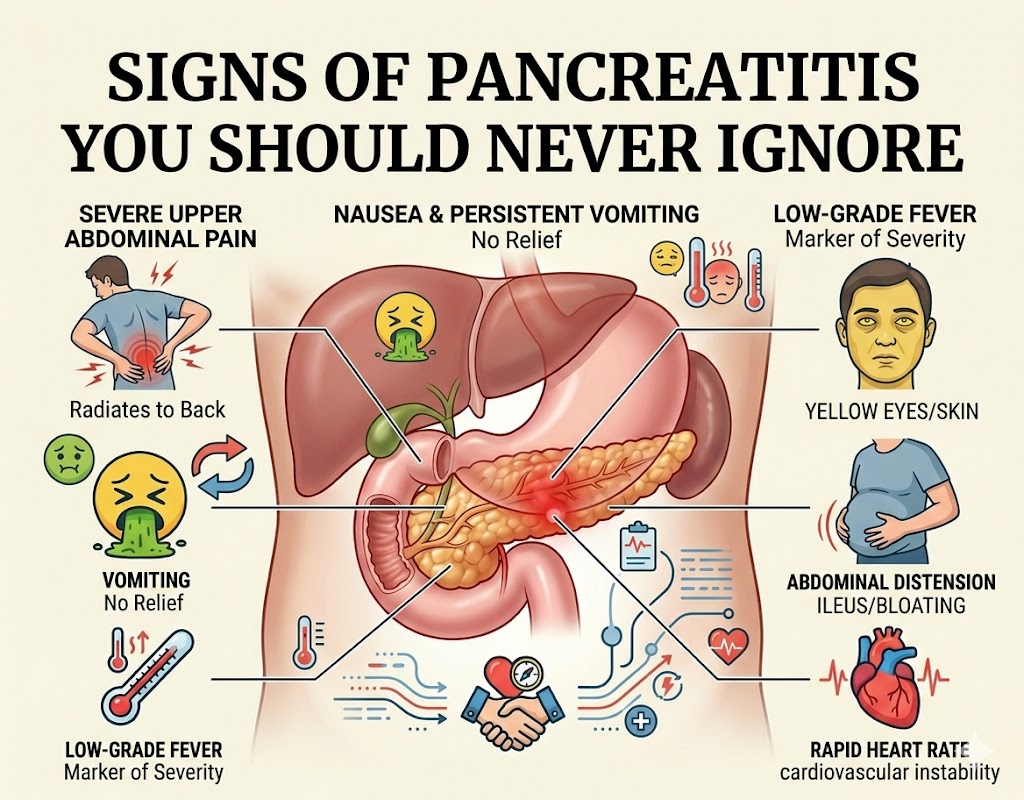
Why Recognizing the Signs of Pancreatitis Matters
Pancreatitis is a medical condition that can escalate from manageable to life-threatening with alarming speed. The pancreas, tucked behind the stomach in the upper abdomen, is not an organ most people think about until something goes wrong with it. But when it becomes inflamed — whether from gallstones, alcohol, medications, or other causes — the consequences can be profound. Recognizing the signs of pancreatitis early is not merely useful; it can be genuinely lifesaving.
Many people who eventually receive a diagnosis of pancreatitis report having dismissed or minimized their early symptoms as ordinary stomach trouble, acid reflux, or muscle strain. This delay in seeking care is dangerous, particularly in acute pancreatitis, where complications such as pancreatic necrosis, organ failure, and sepsis can develop within hours to days. Understanding what the symptoms of pancreatitis look like — and why they occur — empowers you to act quickly and appropriately when they appear.
This comprehensive guide covers every significant sign of pancreatitis you should be aware of, from the most obvious and dramatic to the subtle ones that are frequently overlooked. Whether you are concerned about your own symptoms, caring for someone at risk, or simply educating yourself about this serious condition, the information here will help you recognize the warning signs before they spiral out of control.
The Most Prominent Sign: Severe Upper Abdominal Pain
If there is one symptom that virtually defines pancreatitis, it is severe pain in the upper abdomen. This pain is the cardinal sign of pancreatitis — present in over 95% of cases — and it is unlike most other forms of abdominal pain in several important ways.
The pain of pancreatitis is typically located in the epigastric region — the area just below the breastbone (sternum) and above the navel. It is often described by patients as a deep, boring, or burning sensation. Unlike the cramping pain of gastroenteritis or the colicky pain of kidney stones, pancreatic pain is usually constant and unyielding. It does not come and go in waves; once it starts, it tends to persist without relief.
One of the most distinctive characteristics of pancreatic pain is that it radiates to the back — specifically to the mid-back, between the shoulder blades, or the entire upper back. This radiating pattern occurs because the pancreas lies close to a network of nerve ganglia (nerve clusters), and inflammation in the pancreas irritates these nerves, sending pain signals both forward to the abdomen and backward to the back. Many patients with pancreatitis actually report that their back pain is worse than their abdominal pain — a symptom pattern that should always raise suspicion for a pancreatic cause.
Another tell-tale feature: the pain worsens after eating. Within fifteen to thirty minutes of consuming a meal — especially a fatty, fried, or heavy meal — the pain intensifies, because eating stimulates the pancreas to release digestive enzymes, increasing pressure and inflammation in an already inflamed organ. Conversely, fasting may provide partial relief. Many patients describe finding some relief by sitting up and leaning forward or curling into the fetal position, which reduces the pressure on the inflamed pancreas. If you find yourself instinctively adopting this posture to cope with abdominal pain, it is a significant sign that your pancreas may be involved and you should seek medical care immediately.
Sign Two: Nausea and Persistent Vomiting
Accompanying the abdominal pain in nearly all cases of acute pancreatitis are nausea and vomiting. These symptoms arise from multiple mechanisms: the local inflammatory process in the abdomen, the direct effect of pancreatic inflammation on gastrointestinal motility (the normal movement of food through the digestive tract), and the intense pain itself, which triggers the vomiting center in the brain.
What makes the vomiting of pancreatitis particularly notable — and clinically telling — is that it provides no relief. In conditions like food poisoning, gastroenteritis, or gastroparesis, vomiting often brings at least temporary relief from nausea. In pancreatitis, however, vomiting does nothing to alleviate the pain or nausea. Patients will vomit repeatedly and still feel terrible afterward. This is a critical distinguishing feature. If you are experiencing severe abdominal pain with vomiting that provides no relief, this is a significant warning sign that your pancreas — not your stomach — may be the source of the problem.
Severe and prolonged vomiting in pancreatitis can lead to dangerous dehydration and electrolyte imbalances. Signs of dehydration include extreme thirst, dry mouth, decreased urine output, dark-colored urine, dizziness when standing, and rapid heartbeat. If vomiting is so persistent that you cannot keep any fluids down, you need emergency medical care for intravenous fluid replacement.
Sign Three: Fever — A Marker of Severity
A low-grade fever (between 37.5°C and 38.5°C or 99.5°F and 101.3°F) is a common finding in acute pancreatitis, reflecting the body's systemic inflammatory response to pancreatic injury. In mild pancreatitis, fever is typically modest and short-lived, resolving as the inflammation subsides over the first few days of treatment.
However, a high fever — above 38.5°C (101.3°F) — or a fever that returns after an initial improvement, carries serious significance in pancreatitis. It may signal a secondary bacterial infection, such as infected pancreatic necrosis (bacteria colonizing dead pancreatic tissue) or a pancreatic abscess (a localized collection of pus). Both of these complications require urgent treatment with antibiotics and often drainage procedures. Fever accompanied by chills, rigors (violent shaking), and worsening abdominal pain is a medical emergency that requires immediate evaluation.
Another dangerous cause of high fever in pancreatitis is cholangitis — infection of the bile ducts — which typically occurs when a gallstone obstructs the bile duct and bacteria ascend into the biliary system. Charcot's triad (fever, jaundice, and right upper quadrant pain) and Reynolds' pentad (Charcot's triad plus confusion and low blood pressure) are signs of ascending cholangitis and represent a life-threatening emergency requiring immediate ERCP to clear the bile duct obstruction and IV antibiotics.
Sign Four: Jaundice — Yellow Skin and Eyes
Jaundice — characterized by the yellowing of the skin, whites of the eyes (sclerae), and sometimes the mucous membranes — is a significant sign of pancreatitis, particularly when it is caused by gallstones or when a pancreatic tumor is present. Jaundice occurs when bilirubin, a yellow pigment produced from the breakdown of red blood cells, accumulates in the bloodstream due to obstruction or impairment of its normal excretion into bile.
In gallstone pancreatitis, jaundice develops when a gallstone lodges in the common bile duct and blocks the flow of bile from the liver into the small intestine. In pancreatic cancer, a tumor in the head of the pancreas may compress or invade the bile duct, causing progressive jaundice. In severe acute pancreatitis, swelling of the head of the pancreas can cause extrinsic compression of the bile duct, leading to temporary jaundice.
Associated signs of jaundice from bile duct obstruction include dark brown or tea-colored urine (from bilirubin excreted in the urine), pale, clay-colored, or acholic stools (from absence of bile pigments in the stool), and generalized itching (pruritus) from bile salt deposition in the skin. Any combination of abdominal pain with jaundice, dark urine, and pale stools should be evaluated urgently, as these findings suggest significant bile duct obstruction that requires prompt intervention.
Sign Five: Rapid Heart Rate and Low Blood Pressure
In cases of severe pancreatitis, the body's inflammatory response can cause systemic effects that manifest as cardiovascular instability. A rapid heart rate (tachycardia, defined as a heart rate above 100 beats per minute) and low blood pressure (hypotension, particularly systolic blood pressure below 90 mmHg) are serious warning signs that indicate the pancreatitis is severe and potentially life-threatening.
These signs result from multiple mechanisms: the loss of large volumes of fluid into the abdominal cavity (third-spacing), the widespread vasodilation caused by inflammatory mediators, and the inability of the heart to compensate adequately. Together, these processes can lead to hypovolemic shock — a state in which inadequate blood volume prevents sufficient oxygen delivery to organs and tissues. If untreated, shock can lead to kidney failure, brain damage, and death within hours.
Recognizing these signs requires knowing the warning symptoms: a racing or pounding heart sensation, lightheadedness or dizziness (especially when standing up), feeling faint or actually fainting, cold and clammy skin, and confusion or altered mental status. Any combination of severe abdominal pain with these cardiovascular symptoms demands immediate emergency care.
Sign Six: Abdominal Tenderness and Bloating
During a physical examination, a doctor will typically find significant tenderness on pressing the upper abdomen of a patient with pancreatitis. This tenderness results directly from the inflamed pancreas and the surrounding peritoneal reaction. In severe cases, the abdomen may be rigid or guarded — the patient involuntarily tenses the abdominal muscles to protect the inflamed tissue from palpation — a clinical finding known as involuntary guarding, which indicates peritoneal irritation.
Abdominal distension (bloating and swelling of the abdomen) is common in pancreatitis, resulting from ileus — a temporary cessation of intestinal movement caused by the inflammation spreading to the surrounding intestinal walls. In ileus, gas and fluid accumulate in the intestines because peristalsis (the wave-like muscular contractions that move food along) is suppressed. This causes the abdomen to appear swollen and feel tight, often accompanied by the absence of bowel sounds (no gurgling) or, paradoxically, very high-pitched tinkling sounds on auscultation.
Two rare but significant physical signs associated with severe necrotizing pancreatitis are Cullen's sign and Grey Turner's sign. Cullen's sign refers to bruising (ecchymosis) around the navel, while Grey Turner's sign refers to bruising on the flanks (sides of the abdomen). Both signs result from retroperitoneal hemorrhage — bleeding from the pancreatic bed that tracks along fascial planes to the skin surface. Their presence indicates a severe, hemorrhagic form of pancreatitis with a high mortality rate.
Sign Seven: Steatorrhea — Oily, Foul-Smelling Stools
While not typically a sign of acute pancreatitis, steatorrhea is one of the most telling signs of chronic pancreatitis and exocrine pancreatic insufficiency. Steatorrhea refers to stools that are pale, greasy, oily, unusually bulky, and have a particularly offensive, rancid odor. These stools may float in the toilet bowl, leaving an oily ring on the water surface. They may be difficult to flush and may leave a greasy residue on the inside of the toilet.
Steatorrhea occurs because the pancreas can no longer produce sufficient amounts of lipase — the enzyme responsible for breaking down dietary fats in the small intestine. When lipase output falls below roughly 10% of normal, fat digestion fails, and undigested fat passes through the intestine and appears in the stool. This is actually a late-stage finding, indicating that significant pancreatic exocrine function has already been lost.
Beyond the unpleasant nature of steatorrhea, it has serious nutritional consequences. Undigested fat carries with it fat-soluble vitamins A, D, E, and K, leading to deficiency states over time. Vitamin D deficiency weakens bones (osteomalacia, osteoporosis). Vitamin K deficiency impairs blood clotting. Vitamin A deficiency affects vision and immune function. Vitamin E deficiency can cause neurological and muscular problems. The malabsorption also contributes to weight loss, fatigue, and muscle wasting. If you notice pale, floating, oily stools, discuss this symptom with your doctor — it is a key sign of pancreatic exocrine insufficiency that requires investigation and treatment.
Sign Eight: Unexplained Weight Loss
Unexplained and unintentional weight loss is a warning sign associated with several serious forms of pancreas disease, including pancreatic cancer and advanced chronic pancreatitis. It should never be attributed simply to changes in appetite or stress without proper investigation.
In pancreatic cancer, weight loss is often striking and rapid — patients may lose 10-15% of their body weight over a few months, even when trying to maintain food intake. This occurs due to a complex cancer-related metabolic syndrome called cachexia, which involves not only reduced food intake (from pain, nausea, and loss of appetite) but also abnormal metabolism in which the body continues to break down muscle and fat even when caloric intake is maintained. Cachexia is driven by inflammatory cytokines produced by the tumor and the immune response, and it cannot be reversed simply by eating more.
In chronic pancreatitis, weight loss results from a combination of inadequate caloric intake (patients eat less to avoid triggering pain) and malabsorption (nutrients, especially fats, are not properly digested and absorbed). Over months and years, this leads to progressive muscle wasting, fat loss, and nutritional deficiencies. Addressing weight loss in chronic pancreatitis requires both treating the underlying inflammation and optimizing nutritional support, including pancreatic enzyme replacement.
Sign Nine: New-Onset Diabetes or Worsening Blood Sugar Control
The pancreas produces insulin, the hormone that enables cells to absorb and use glucose from the bloodstream. When pancreatic tissue is damaged — through chronic inflammation, surgical removal, or tumor invasion — insulin production falls, and blood sugar levels rise. This results in a specific form of diabetes known as Type 3c diabetes or pancreatogenic diabetes.
New-onset diabetes — particularly in individuals over 50 who have no family history of diabetes, who are not obese, and who have not previously had blood sugar problems — is a red flag that may indicate underlying pancreatic disease, including early pancreatic cancer. Research shows that approximately 1% of patients with new-onset diabetes over age 50 have an underlying pancreatic cancer that is driving the blood sugar dysregulation. While this is a small percentage, it is significant enough that unexplained new-onset diabetes in older adults warrants pancreatic imaging to rule out a tumor.
In established chronic pancreatitis, the development of diabetes indicates that endocrine pancreatic function has been significantly impaired. Pancreatogenic diabetes is more complex to manage than Type 1 or Type 2 diabetes because the absence of glucagon (which is also produced by the damaged pancreas) makes patients highly susceptible to hypoglycemia (dangerously low blood sugar), particularly when insulin doses are not carefully calibrated.
Sign Ten: Itchy Skin (Pruritus)
While less well-known than pain or jaundice, itchy skin (pruritus) can be a significant sign of pancreatitis-related bile duct obstruction. When bile cannot flow normally from the liver into the intestine because the bile duct is blocked or compressed, bile salts accumulate in the bloodstream and deposit in the skin. This causes an intensely uncomfortable, generalized itching that is often worse at night and not relieved by scratching or topical treatments.
Pruritus associated with jaundice in the context of pancreatitis is a sign of obstructive jaundice and should prompt urgent evaluation for bile duct stones, strictures, or compression from a pancreatic mass. Treatment of the underlying obstruction — whether by ERCP, percutaneous drainage, or surgery — typically resolves both the jaundice and the pruritus.
Signs That Require Immediate Emergency Care
While all signs of pancreatitis merit medical attention, certain combinations demand emergency care without any delay. Call emergency services or go immediately to the nearest emergency department if you or someone you are with experiences any of the following: severe, sudden-onset upper abdominal pain that is the worst pain ever felt; abdominal pain with fever above 38.5°C or 101.3°F, chills, and rapid heart rate; abdominal pain with jaundice (yellow skin or eyes); vomiting blood or passing black, tarry stools (melena); signs of shock including dizziness, confusion, cold clammy skin, or fainting; and rigid, board-like abdomen with extreme tenderness. These are all potential indicators of severe pancreatitis or its life-threatening complications and require immediate evaluation and treatment.
When to Seek Non-Emergency but Prompt Medical Care
Certain symptoms of pancreatitis do not constitute immediate emergencies but still require prompt medical evaluation within days rather than weeks. These include persistent upper abdominal or back pain that has lasted more than two to three days, pale or oily stools suggesting exocrine insufficiency, unexplained weight loss of five percent or more over a few months, new-onset or worsening diabetes without other explanation, recurrent episodes of abdominal pain especially after meals or alcohol, and a family history of pancreatitis combined with any of the above symptoms. Do not dismiss or delay evaluation of these symptoms. Chronic or recurrent pancreatic conditions are most effectively managed when caught and treated early.
Conclusion: Listen to What Your Body Is Telling You
The signs of pancreatitis are your body's urgent communication that something serious is happening in your abdomen. From the unmistakable severity of upper abdominal pain radiating to the back, to the subtler warnings of oily stools, unexplained weight loss, and new-onset diabetes — these symptoms deserve to be heard, taken seriously, and acted upon promptly.
Pancreatitis does not distinguish between age groups, genders, or lifestyles. It can affect anyone, from a young adult after their first bout of heavy drinking to a middle-aged woman with previously undetected gallstones, to an elderly man whose new-onset diabetes turns out to be the first sign of pancreatic cancer. The common thread is that those who recognize the signs early and seek timely medical care have significantly better outcomes than those who wait.
If you recognize any of the symptoms described in this guide — especially in combination — do not rationalize them away. Seek medical evaluation. A blood test, an ultrasound, or a CT scan taken promptly can mean the difference between a manageable episode of pancreatitis and a life-threatening complication. Your health is worth the urgency.